Filing a VA claim for autoimmune diseases like lupus or rheumatoid arthritis can seem challenging. But support is available. This guide will walk you through the process step-by-step.
We’ll cover gathering evidence, submitting your disability claim, and understanding the VA system. By the end, you’ll have a clearer path for getting the disability benefits you earned through your military service.
Autoimmune diseases can significantly impact your daily function. These conditions happen when your immune system mistakenly attacks your body’s healthy tissue. For veterans, autoimmune disorders may be linked to events or exposures during active duty or active duty training.

Understanding Autoimmune Diseases and VA Claims
Let’s discuss autoimmune diseases before getting into the VA disability claim process. Conditions like systemic lupus erythematosus (SLE), rheumatoid arthritis, Sjogren’s syndrome, myasthenia gravis, and multiple sclerosis fall under this category. They can cause symptoms ranging from joint pain and swelling (common in arthritis va cases) to extreme fatigue and organ damage.
An autoimmune disorder occurs when the immune system fails to distinguish between the body’s own cells and foreign invaders. Instead of only attacking bacteria or viruses, it starts to produce antibodies that target healthy tissue. This attack causes inflammation and damage, leading to the symptoms of the specific autoimmune disease.
The Department of Veterans Affairs (VA) recognizes many commonly-recognized autoimmune diseases as potentially service-connected disabilities. This means you might qualify for VA disability compensation if your autoimmune disorder is related to your military service. Establishing this service connection is critical, but it can require detailed proof, making it essential to know how to build a strong va disability claim.
Step 1: Gather Your Medical Evidence
The initial step in filing your VA claim is gathering comprehensive medical evidence. This documentation is vital for proving your diagnosis and establishing the necessary link military service connection. Your evidence file should ideally contain:
- Complete medical records confirming your autoimmune disease diagnosis (e.g., lupus erythematosus, rheumatoid arthritis).
- Detailed treatment records, including medications, therapies, and doctor visits related to your autoimmune condition.
- Results from laboratory tests, imaging studies (X-rays, MRIs), and biopsies.
- Written statements or medical opinions from your treating physicians detailing your condition, its severity, and its impact on your life. These are often called Independent Medical Opinions (IMOs) or Nexus Letters.
Remember to include any relevant service treatment records (STRs). These records from your time in service can be critical for showing when symptoms first began or if an event during active duty might have contributed to your condition. STRs document any medical care received while on active duty or active duty training.
If you find gaps in your medical records, you can formally request copies from the VA healthcare system, military medical facilities, or your private healthcare providers. Diligence in collecting all available medical evidence strengthens your disability claim considerably. Thorough documentation forms the backbone of successful disability claims.

Step 2: Connect Your Condition to Your Service
Establishing the service connection is often the most challenging aspect of a VA disability claim for an autoimmune disease. You need to demonstrate that your military service caused or aggravated your condition. There are several ways the VA may grant service connection:
- Direct Service Connection: Provide evidence that your autoimmune disease began during service or was caused by a specific event, injury, or exposure during service. This might involve showing symptoms documented in your STRs or linking exposure to known environmental hazards like Agent Orange or burn pits.
- Secondary Service Connection: Show that your autoimmune disease was caused or aggravated by another service-connected condition. For example, if you have a service-connected joint injury that later contributed to the development of rheumatoid arthritis in that joint.
- Presumptive Service Connection: Certain autoimmune diseases may be presumed service-connected if you served in specific locations during particular periods (e.g., Vietnam veterans exposed to Agent Orange, Gulf War veterans, Afghanistan veterans exposed to burn pits). For instance, some conditions associated with Gulf War syndrome are recognized presumptively. The VA maintains lists of conditions presumed linked to certain exposures or service eras.
- Aggravation: Demonstrate that your military service worsened a pre-existing autoimmune condition beyond its natural progression. This requires medical evidence showing the condition existed before service and worsened due to service.
Gathering supporting evidence is key. This can include:
- Military personnel records documenting exposure to specific environmental factors (e.g., deployment orders, job descriptions indicating work near burn pits).
- Scientific or medical studies linking certain exposures (like Agent Orange or contaminants from burn pits) to the development of specific autoimmune diseases.
- Buddy Statements: Written statements from fellow service members who can attest to your symptoms starting during service, or exposure incidents.
- Lay Statements: Your own detailed account of your symptoms, their onset, progression, and impact on your life, as well as any relevant service events.
If your autoimmune disease symptoms appeared within one year of discharge from active duty, the VA might grant presumptive service connection for certain chronic conditions. Even if more time has passed, a strong link military service case can still be made with compelling medical evidence and lay testimony. Do not be discouraged if your diagnosis came years after service; focus on building the connection.
Step 3: Fill Out the Right Forms
Next, you must complete the necessary application forms. The primary form for initiating a disability claim is VA Form 21-526EZ, Application for Disability Compensation and Related Compensation Benefits. You can download this form directly from the VA website or complete it online.
Accuracy and detail are vital when filling out the form. Clearly list your diagnosed autoimmune disease(s), such as systemic lupus erythematosus or rheumatoid arthritis. Describe all related symptoms and explain how they limit your ability to work and perform daily activities.
Do not minimize the severity or frequency of your symptoms or how exacerbations occur. The VA needs a clear picture of the full impact your service-connected condition has on your functionality. Include details about pain levels, fatigue, mobility restrictions, and any effects on mental health.

Step 4: Submit Your Claim
After assembling your medical evidence, supporting documents, and completed forms, it’s time to submit your VA disability claim. You have several options for submission:
- Online: Use the VA.gov website. This method is generally the fastest and allows for easy tracking.
- Mail: Send your completed application package to the VA Evidence Intake Center address listed on the form. It’s wise to use certified mail for tracking.
- In Person: Deliver your claim documents to a VA Regional Office.
Regardless of the method chosen, always keep complete copies of everything you submit for your records. Confirming receipt by the VA is also a good practice. Submitting online often provides immediate confirmation.
Step 5: Attend Your C&P Exam
Once the VA receives your claim, they will review the submitted evidence. They will likely schedule you for one or more Compensation and Pension (C&P) examinations. Attending these appointments is mandatory; failure to attend without a valid reason can result in claim denial.
The C&P exam is a medical evaluation conducted by a VA doctor or a VA-contracted physician. The purpose is to assess the severity of your claimed condition(s) and gather medical evidence to help the VA rater make a decision on your disability claim. The examiner will review your file, ask questions about your condition and history, and perform a physical examination.
Preparation for the C&P exam is important:
- Review your medical records and submitted documents beforehand.
- Make notes about your symptoms, including frequency, duration, and severity, especially focusing on how they impact your daily life and work ability. Be specific about limitations (e.g., difficulty walking distances, trouble gripping objects, needing rest periods due to fatigue).
- Be completely honest and open with the examiner. Describe your symptoms accurately – do not exaggerate, but also do not downplay your pain or limitations. Explain how your condition affects you on both good and bad days.
- Bring copies of any relevant private medical records that the VA might not have received yet.
Understand that the C&P examiner’s role is evaluation, not treatment. They will produce a report summarizing their findings, which becomes part of your claim file. You have the right to request a copy of the C&P exam report after it’s completed.
Step 6: Follow Up on Your Claim
Following your C&P exam, a VA rating specialist will review all the evidence, including the examiner’s report, your medical records, service records, and any lay statements. They will then make a decision regarding service connection and assign a disability rating if applicable. This process can take several months or longer, depending on claim complexity and VA workload.
You can monitor the status of your VA disability claim online through your VA.gov account or by calling the VA’s toll-free number (1-800-827-1000). Checking periodically allows you to see if the VA requires any additional information.
Understanding VA Disability Ratings for Autoimmune Diseases
If the VA grants service connection for your autoimmune disease, they will assign a disability rating. The VA assigns disability ratings based on the severity of your symptoms and how much they impact your ability to work and function. Ratings are expressed as percentages, typically ranging from 0% to 100% in increments of 10.
The VA uses the VA Schedule for Rating Disabilities (VASRD) to determine the appropriate percent disability. Autoimmune diseases are rated under various diagnostic codes depending on the specific condition and the body systems affected. For example:
- Systemic Lupus Erythematosus (SLE): Rated under Diagnostic Code 6350. The VA assigns a disability rating based on the frequency and severity of exacerbations (flare-ups) and constitutional symptoms like fatigue, fever, and weight loss. Ratings can be 100% during periods requiring high-dose corticosteroids or immunosuppressants, 60% for frequent exacerbations occurring several times a year, 30% for exacerbations occurring less frequently, or 10% for less severe cases.
- Rheumatoid Arthritis: Typically rated under Diagnostic Code 5002. Ratings depend on the number of joints affected, limitation of motion, frequency of flare-ups, and systemic effects. Severe cases involving incapacitating episodes or significant joint deformities can receive higher ratings, potentially up to 100%.
- Discoid Lupus: Rated under Diagnostic Code 7809, based on skin lesions and scarring.
- Sjogren’s Syndrome: Rated based on the body systems affected (e.g., dry eyes under eye conditions, dry mouth under dental issues, joint pain under arthritis).
- Myasthenia Gravis: Rated under Diagnostic Code 8025, based on severity of muscle weakness affecting functions like breathing, swallowing, vision, and movement. Ratings range from 10% to 100%.
The VA assigns disability ratings based on the evidence provided. If multiple body systems are affected by an autoimmune disease like lupus severe enough to warrant separate ratings, the VA uses a combined rating table to calculate the overall disability percentage. Frequent exacerbations often lead to higher disability ratings because they significantly disrupt daily life and work.
It’s important to provide detailed evidence about how often exacerbations occur and how severe they are. Keeping a symptom journal can be helpful medical evidence. Understanding how the VA assigns disability ratings helps you present the most relevant information in your claim.
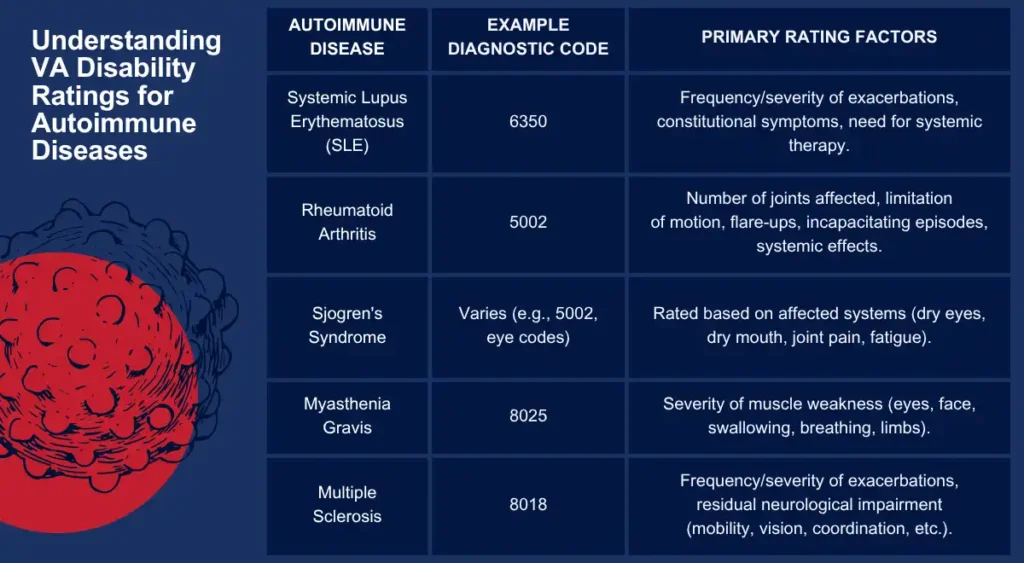
Note: This table provides general examples. The specific diagnostic code and rating criteria depend on the individual case and the current VASRD regulations.
What to Do If Your Claim Is Denied
Receiving a denial for your VA disability claim can be disheartening, but it is not the end of the road. You have the right to appeal the decision. The VA modernized its appeals process, offering several options:
- Supplemental Claim: Submit new and relevant evidence that was not previously considered by the VA. This is often the best option if you have new medical records or reports that strengthen your case. (VA Form 20-0995)
- Higher-Level Review: Request that a senior VA reviewer re-examine your case based on the existing evidence. No new evidence can be submitted with this option. (VA Form 20-0996)
- Board Appeal: Appeal directly to the Board of Veterans’ Appeals (BVA). You can choose one of three dockets: direct review (no new evidence, no hearing), evidence submission (submit new evidence), or a hearing with a Veterans Law Judge. (VA Form 10182)
Understanding why your claim was denied is crucial for choosing the right appeal path. The VA decision letter will outline the reasons for denial. Review this information carefully.
Tips for a Successful VA Claim
Filing a VA claim for autoimmune diseases requires careful preparation and persistence. Here are some tips to improve your chances of a successful outcome for receiving VA disability benefits:
- Be Thorough: Provide comprehensive medical evidence and detailed statements about your condition and its connection to service. Include all relevant diagnoses, like diabetes mellitus type I if applicable, as it’s also an autoimmune disorder.
- Meet Deadlines: Pay close attention to all deadlines for submitting forms, evidence, and appeals. Missing a deadline can jeopardize your claim.
- Be Honest and Consistent: Accurately describe your symptoms and limitations during exams and in your statements. Consistency across your records and testimony is important.
- Document Everything: Keep copies of all submitted documents, correspondence with the VA, and medical records. Maintain a log of communications.
- Understand Secondary Conditions: Autoimmune diseases can cause other health problems. File claims for these secondary conditions if they arise (e.g., depression secondary to chronic pain from rheumatoid arthritis).
- Consider TDIU: If your service-connected autoimmune disease(s) prevent you from maintaining substantially gainful employment, even if your combined rating is less than 100%, you may be eligible for Total Disability based on Individual Unemployability (TDIU). This pays at the 100% disability rate.
- Be Persistent: The VA claims process can be long and sometimes frustrating. If your initial claim or appeal is denied, review the decision, gather more evidence if possible, and continue pursuing the VA benefits you deserve. Social Security disability benefits are separate but having VA documentation can sometimes assist with that process too.
Remember, proving service connection for an autoimmune disease involves showing the link military service had to your current condition. This might involve evidence from your active duty time, including duty training records, or linking it to specific exposures known to cause autoimmune responses. The VA system is there to provide support, and persistence often pays off.

Conclusion
Filing a VA claim for autoimmune diseases such as lupus erythematosus or rheumatoid arthritis demands thoroughness and patience. Obtaining VA disability compensation acknowledges the sacrifices made during military service and provides essential support. By following these steps, diligently gathering medical evidence and proof of service connection, and understanding the VA processes, you can improve your chances of success.


